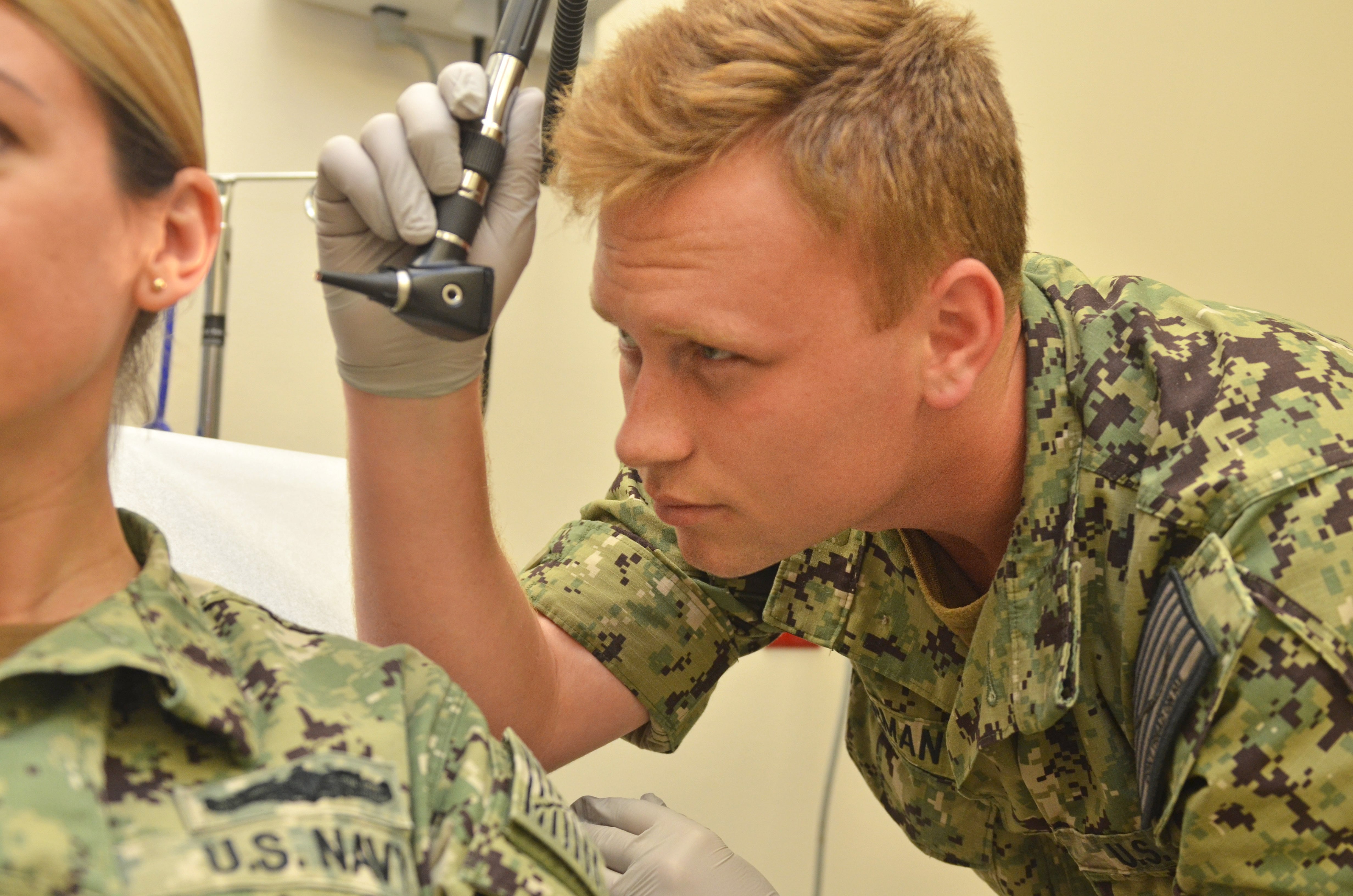
The Pentagon’s fiscal 2021 budget request supports ongoing, sweeping changes to the military health system that will reduce the number of uniformed medical personnel and send non-active duty beneficiaries to contractors or civilian providers for their health care.
The $50.8 billion proposed Department of Defense medical budget released Monday continues reforms initiated in 2017 that place the service medical commands in charge of providing health care for uniformed personnel and gives oversight and responsibility of all military hospitals and clinics to the Defense Health Agency, to include staffing decisions.
According to the budget documents, this means some non-uniformed beneficiaries — active-duty family members, retirees and their family members — will continue receiving care at military treatment facilities from civilian staff or contractors, while others, “where feasible …. will be transitioned to a local network provider.”
The budget documents affirm what Defense Health Agency officials have said for months: the military health system must right-size the military medical forces to support operational medicine, while roughly 8 million non-uniformed beneficiaries will receive health care from civilian federal employees, contract care or in the community, via Tricare.
RELATED

In some locations, such changes are underway. In the past two years, military hospitals at Fort Knox, Kentucky; Fort Jackson, South Carolina; and Fort Sill, Oklahoma, were downgraded to outpatient clinics, a reconfiguration that resulted in retirees, retiree family members and some active duty family members transferring to physicians off-base.
Military.com reported Friday that commanders of 50 military treatment facilities targeted for changes received a memo from Defense Health Agency officials detailing the changes, which could affect at least 200,000 beneficiaries.
According to the report, non-uniformed beneficiaries currently enrolled at 38 military hospitals nationwide will be forced to go off-base.
The details are spelled out in a report expected to go to Congress in the coming weeks.
“It is estimated that approximately 200,000 Military Health System beneficiaries who receive care at the MTFs identified for reduction in operations will transition to civilian providers” in the Tricare network, Military.com reported.
Military advocates and members of Congress have raised concerns over the impact of transferring military beneficiaries to community providers in locations where there are not enough doctors or specialty services or in areas where services are unavailable.
At a Defense Health Board meeting Monday, a DHA official said in some remote places, such as Twentynine Palms, Calif., hospitals will continue caring for all beneficiaries since services aren’t available in the surrounding communities.
The fiscal 2021 budget request of $50.8 billion is a decrease of 1.2 percent from the fiscal 2020 enacted level, with the cuts coming mainly from the elimination of nearly $1.6 billion in research funding added each year to the Pentagon budget by Congress as part of the Congressionally Directed Medical Research Program.
Each year in its budget proposal, the Pentagon lines out CDMRP and Congress adds the dollars back in, to fund research projects that members have deemed necessary to preserve the health of the armed forces. CDMRP research currently includes certain types of cancer, autism, tick-borne diseases, Alzheimer’s and more.
The budget also proposed to transfer several medical readiness activities and functions to the military services deemed outside the scope of the Defense Health Agency, although the documents did not provide specifics.
RELATED
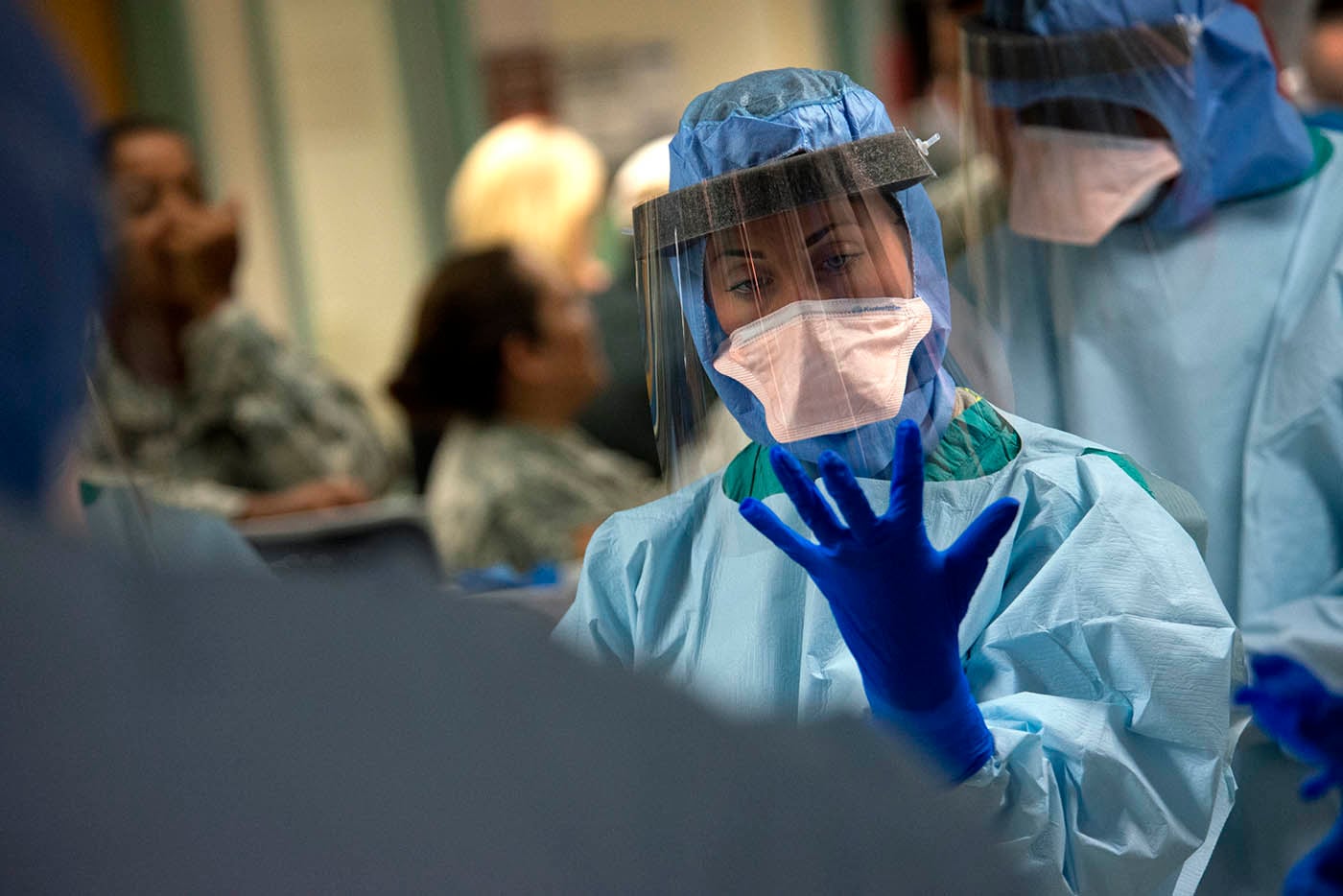
Defense health officials say their goal with the transformation is to maintain a healthy force, a military medical staff focused on operational medicine and an improved health care system for non-military beneficiaries.
But for those forced off-base to receive medical care, the transition will come with an additional financial burden. Currently, beneficiaries who receive care at military hospitals or clinics have no co-payments for services or prescriptions.
But in the community, retirees and their family members enrolled in Tricare Prime can expect co-pays ranging from $20 for an outpatient primary care appointment to $62 for an emergency room visit, while those who choose Tricare Select will pay between $30 for a network primary care appointment up to $118 for a network emergency room visit.
Prescription co-payments outside military pharmacies range from $10 for home delivery of generic medications to $60 for a medication not listed on Tricare’s formulary at a network retail pharmacy.
The proposed fiscal 2021 proposed $4.8 trillion White House budget designated nearly $741 billion for defense spending, including a 3 percent pay raise for military personnel.
Patricia Kime is a senior writer covering military and veterans health care, medicine and personnel issues.