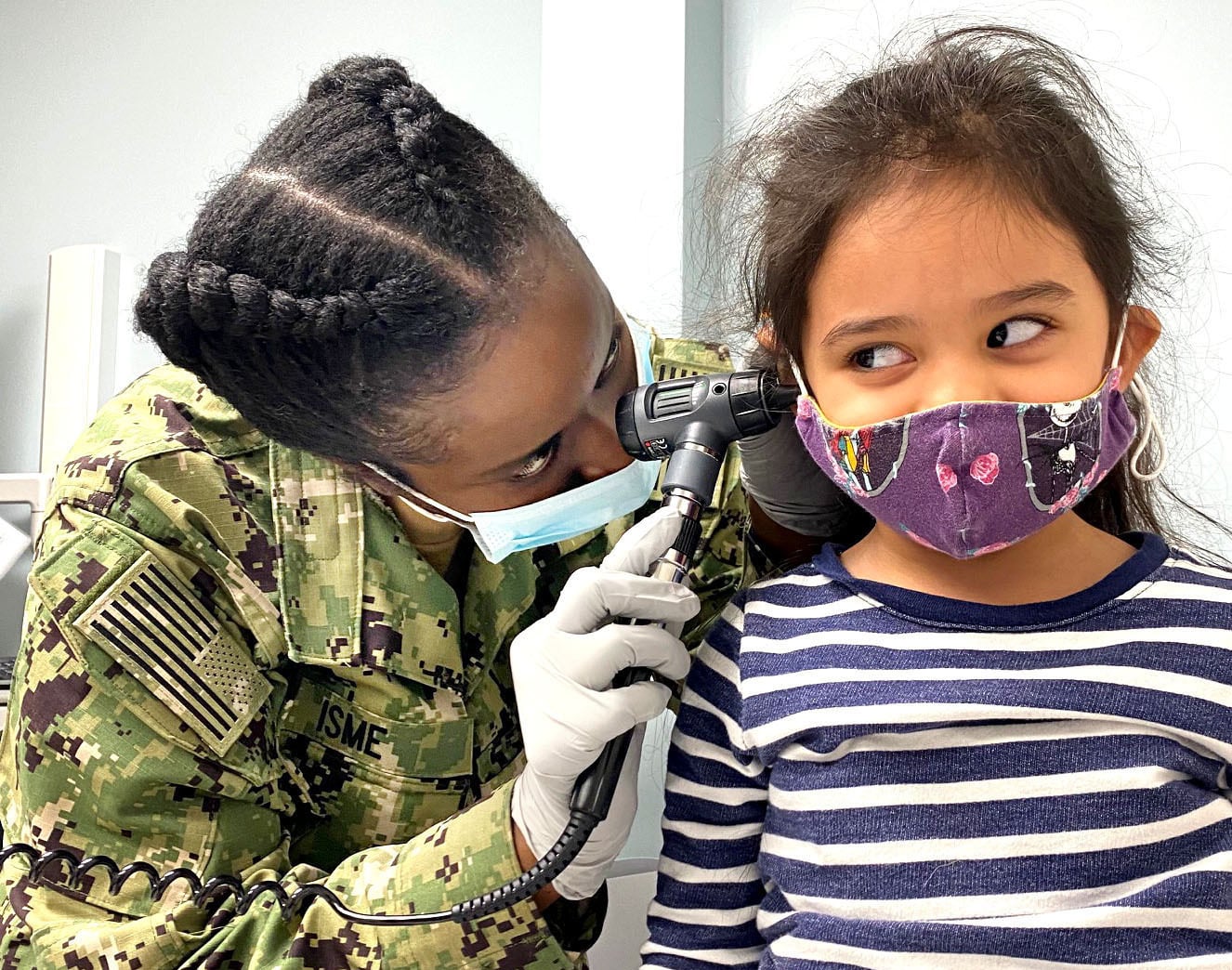
After years of forcing some military beneficiaries to seek medical care in the private sector, the Defense Department wants to attract patients back to military treatment facilities.
Citing problems that have led to “chronically understaffed military treatment facilities and dental treatment facilities,” Deputy Secretary of Defense Kathleen Hicks has directed sweeping changes to boost staffing at medical facilities and increase access to care for beneficiaries.
“Our service members, their families, other beneficiaries and all those cared for by military medicine will be better served when we rebuild [military treatment facility] capacity,” Hicks wrote in a Dec. 6 memo entitled “Stabilizing and Improving the Military Health System.”
Hicks laid out a plan to grow the number of patients who receive care in a military treatment facility by 7% by the end of 2026, compared to the number of beneficiaries in December 2022. That would mean 3.3 million people would be using the MTFs in three years, according to Military Times calculations.
About 9.5 million beneficiaries are part of the military health system.
The push is driven by concerns about medical readiness as well as cost, Hicks said. DOD’s overall health care costs have risen as patients have migrated to the civilian sector. That decline in patients has also spurred the military services to seek private-sector training opportunities to keep their medical staff’s clinical skills current.
For more than a year, stakeholders from patients to military medical providers to military leaders have reported myriad issues stemming from medical personnel shortages that have led to patients being unable to get the care they need, or delays in that care.
If DOD loses more patients to the civilian medical system, military beneficiaries could face “significantly worse” surgical mortality rates, medical mortality rates and patient safety than in military treatment facilities, one Pentagon-funded study found.
Hicks’ memo came a week after a Nov. 29 Defense Department Inspector General report detailing how beneficiaries around the world have dealt with military medical provider shortages, few civilian network options and long wait times. The Defense Health Agency did not respond to the Pentagon watchdog’s recommendations.
RELATED
The Defense Department had planned to cut military medical billets before the coronavirus pandemic began. Congress put the brakes on that effort in the fiscal year 2023 National Defense Authorization Act, halting the plan for five years, and requiring a series of reports before any cuts are made.
The military health system has undergone a massive reorganization over the past four years, moving military clinics and hospitals under the Defense Health Agency’s control rather than that of the service branches.
To do so, Hicks noted, DOD “adopted a complex approach to managing the medical workforce.”
She acknowledged that the realignment of medical personnel, the challenging national health care economy, and DOD’s “ambitious private-sector care capacity assumptions” led to chronically understaffed medical and dental treatment facilities that, at times, can’t deliver timely care. Nor can they ensure that there’s a sufficient workload to maintain medical providers’ clinical skills, she said.
To attack the problem, DOD convened subject matter experts from across the department who decided the best solution is to convince beneficiaries to return to the MTFs and to maximize the medical education and training pipelines.
But getting people to return to their military doctors and dentists “requires a stable, predictable workforce sufficiently staffed, trained, and routinely available to provide health care to our beneficiaries,” Hicks said.
That has raised concerns among some family advocates.
“It seems like the plan is to simultaneously recapture beneficiaries while also still working out how to manage the medical work force across DOD and the services,” said Karen Ruedisueli, director of government relations for health affairs for the Military Officers Association of America.
“Looking at the memo, I’m concerned that they don’t yet have a proven approach to address the MTF staffing problem, yet there’s a recapture goal out there” to bring 7% of health care back to those facilities, she said. “Where does that 7% come from, and where do they go? Where are they going to go within the system that has acknowledged problems with staffing?”
“This could turn into a real recipe for problems with access to care for military families,” she added.
Increasing access
DOD officials don’t plan to ask any patients to change their health plan or their doctor, the department said in a release.
“The goal is to make the [Military Health System] more accessible, to make getting care at military hospitals or clinics the easiest, simplest choice,” officials said.
The five-page memo outlines steps DOD is taking to hit its goal. The undersecretary of defense for personnel and readiness is conducting a comprehensive review of all medical manpower and staffing, to include active duty, Guard and Reserve, civilian employees and contractors in military treatment facilities and dental facilities, operational units and other areas.
The director of the Defense Health Agency will identify the capacity of each military treatment facility and dental treatment facility to maintain the clinical readiness of active duty health care personnel. By June 30, and annually going forward, the director will assess and set military and civilian manpower requirements for each military medical and dental facility.
DOD will also rethink how it assigns military medical personnel to hospitals and clinics. The department plans to shuffle medical personnel to boost capacity at a few key locations by July 1, officials said.
“We’ll begin PCSing a number of health care professionals,” David Smith, deputy assistant secretary of defense for health readiness policy and oversight, said in the release.
Smith is leading the task force in charge of implementing the memo’s directives. “From there, we’re going to a phased progression of assigning these providers to military hospitals and clinics,” he said.
Assigning military medical forces primarily to military hospitals and clinics increases the predictability and continuity for patients, as well as capacity for day-to-day health care, he said.
Since Jan. 1, the undersecretary of defense for personnel and readiness has been required to have a process for notifying the Defense Health Agency when uniformed medical or dental personnel will be unavailable at military facilities because of operational or readiness requirements, according to Hicks’ memo.
They’ll also implement authorities that allows the Pentagon to better recruit and retain civilian medical staff.
Lester Martinez-Lopez, the DOD assistant secretary for health affairs, also acknowledged the problems in a message to those in the military health system.
“I hear you. I know we have serious issues, and we have a plan to fix our situation. I am asking for your support during the time it will take to make the changes we need,” he said.
More possible fixes
Ruedisueli suggested several other steps defense officials could take to help military families, including a possible pilot program allowing them more flexibility in switching Tricare plans. That could help families navigate the limited capacity plaguing some military treatment facilities and civilian providers who accept Tricare insurance, she said.
“Beneficiaries really need to be able to switch plans to get the appointments that are available, and right now they can’t do that except in the annual open enrollment period,” Ruedisueli said.
For example, if a family in a Tricare Prime plan can’t get appointments at their military treatment facility, they aren’t able to switch to Tricare Select, which offers providers in the local civilian community. Similarly, if they’re in Tricare Select and the local civilian providers can’t meet their needs, they can’t switch to Tricare Prime to seek care at a military treatment facility.
Defense Health Agency officials also need to establish a digital system that allows families to report problems with access to care, such as having difficulty making an appointment, Ruedisueli said. Such a system could help beneficiaries make appointments while adding transparency and flagging problems to officials, she said.
“We know the military health system is committed to delivering beneficiary care, but they can’t fix problems they don’t know about. We need a system that allows families to raise those problems when they occur,” she said.
Karen has covered military families, quality of life and consumer issues for Military Times for more than 30 years, and is co-author of a chapter on media coverage of military families in the book "A Battle Plan for Supporting Military Families." She previously worked for newspapers in Guam, Norfolk, Jacksonville, Fla., and Athens, Ga.